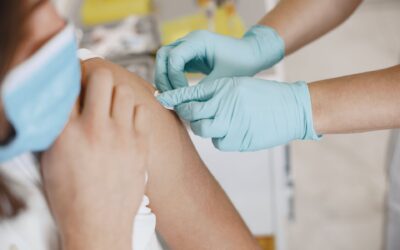
Flu Shots are In! Regular dose flu shots are an included benefit of your Baskin Clinic membership. Call us to schedule an appointment, or get one at...
All the latest
Baskin Clinic Blog
Baskin Clinic Update 7/13/23:
AMA changes BMI to BF%, hip:waist, genetic factor The American Medical Association has made a major policy change in assessing obesity. In addition...
Baskin Clinic Update 4/3/23: Changes to the Mask Mandate, a New Location, and Pharmacy Updates
Mask Policy Change As of today, April 3rd, Oregon is lifting the mask mandate in medical settings. At the Baskin Clinic, this will mean that...
Baskin Clinic Update 8/12/22: Vitamin D Debunked, Monkeypox Vaccines, Paxlovid, and More
Vitamin D Supplements For many years, the assumption has been that supplementing vitamin D would improve health in all the areas of the body where...
Baskin Clinic Update 4/7/22: Living with COVID
We may be done with COVID, but it’s not done with us. There are new (sub)variants to pay attention to, and it’s not clear how this may manifest in...
Baskin Clinic Update 12/23: Threat Level Omicron
Anyone Who is Eligible for Another Dose of COVID Vaccine Should Make Plans to Get it as Soon as Possible. This Includes: Anyone 16+ who received...